I see GERD quite often and many people ask me how I tackle it. In this article I’ll explain my approach to treating GERD so you don’t have to suffer so much!
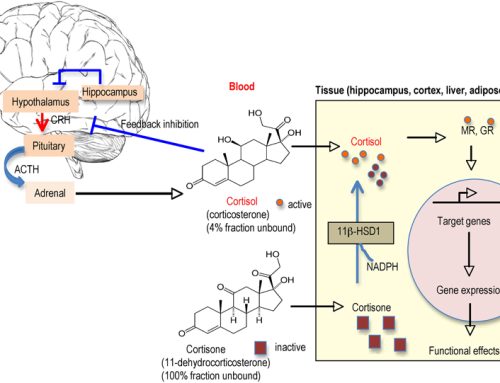
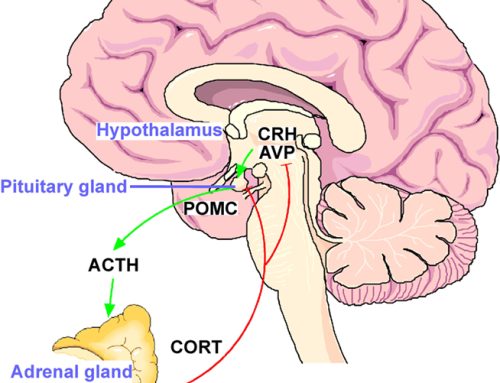
Why does Gastroesophageal Reflux Disease (GERD) happen? After you chew and swallow food it enters the esophagus and then passes through the gastroesophageal sphincter into the stomach. Normally, the gastroesophageal sphincter displays a relatively high pressure that prevents the reflux of stomach contents into the esophagus. However, changes or decreases in the gastroesophageal sphincter pressure can ultimately result in GERD.
But, before we dig deeper into GERD, how do you know it’s GERD or not SIBO (small intestinal bacterial overgrowth) or a peptic ulcer? There are difference in symptoms and treatment of GERD versus SIBO or peptic ulcers.
GERD
- Excessive burping & gas
- Stomach pain, burning, aching 1 – 4 hours after eating
- Heartburn lying down
- Reflux even when not eating
- Alcohol worst contributor
- Worse with acidic food: Coffee, tomato, acids mild
- Better with alkaline foods, antacids and proton-pump inhibitors
- Treated with:
- Lifestyle: High protein, lower carb, lower fat diet; Stress Reduction; Sleep
- Improve lower esophageal sphincter function
- HcL replacement (use code DRMOLLY) if hypochlorhydria (see protocol below to find out if you are a candidate)
SIBO
- Excessive burping & gas
- Bloated after meals
- Recent antibiotics
- Coated tongue
- Alternating stool consistency ranging from constipation to diarrhea
- Often contributes to GERD
- Can be due to Hydrogen dominant or Methane dominant bacterial overgrowth (best to get a breath test to figure this out).
- Treated with
- Antibiotics: Rifaximin (xifaxan) 550 mg TID x 10-14 days
- OR, herbal antibiotics:
- Hydrogen SIBO (Berberine containing herbs – 5000 mg/day; Optionally add Neem – 300 mg TID &/or Oregano – 50 mg TID)
- Methanogenic SIBO (Allicin extract – 450 mg TID for 30 days or 900 mg TID for 10 days; Optionally add Neem – 300 mg TID)
- Prokinetics (erythromycin) can also be an option for 90 days
- Low carb, low fodmap diet
- Supplements: HcL replacement if hypochlorhydria (see hcl protocol to find out if you are a candidate); enzyme replacement for pancreatic insufficiency (use code DRMOLLY for a discount).
Ulcer
- Excessive burping & gas
- Bloated after meals.
- Pain aggravated by meals (may suggest gastric ulcers).
- Heartburn lying down
- Stomach pain, burning, aching 1 to 4 hours after eating
- No dark or tarry stools makes it less likely to be a bleeding ulcer
- Could be due to: Aspirin or NSAIDS which can cause peptic ulcer; H. Pylori (bacteria that causes ulcers).
- Treated with
- Triple therapy: Bimuth + 2 antibiotics OR Proton Pump Inhibitor + 2 antibiotics
- Supplements: Mastic gum, DGL, Vitamin C, Garlic, Berberine, Olive leaf
How Do We Address GERD?
To address GERD, we first need to reexamine some of the behaviors and the foods that influence gastroesophageal sphincter pressure, that may promote increased acid production, and that may irritate an inflamed esophagus. Here are some recommendations for GERD that can help you heal:
- Reduce carbohydrates in the diet (excess abdominal gas can decrease LES pressure).
- The number one thing I do is address diet. I have been able to reverse many cases of GERD by changing a patient’s diet and eliminating refined carbohydrates and sugar as well as grains and legumes (people can always re-introduce these later to see which ones they tolerate).
- There is evidence to suggest high carb diets create more fermentation in the gut creating increased pressure in the stomach leading to reflux of the lower esophageal sphincter. There is published research on higher carb diets being associated with more GERD.
- Increase protein which raises LES pressure.
- Protein is a nutrient that increases gastroesophageal sphincter pressure.
- A higher-than-normal protein intake is encouraged (1.6 g/kg would be ideal especially when weightlifting).
- You may want to focus on lean protein and fish as fatty cuts may aggravate GERD.
- Try to avoid activities that increase in abdominal pressure.
- Eating large meals increases gastric volume.
- Bending, lying down places of gastric contents near the sphincter.
- You should do activities that decrease abdominal pressure.
- Eat smaller meals.
- Eat till 80% full then stop.
- Drink fluids between meals, instead of with a meal, to help minimize large increases in gastric volume.
- In addition, avoid substances that decrease LES sphincter pressure, which is already low because of the condition.
- Several substances decrease gastroesophageal sphincter pressure, including high-fat foods (e.g., fried food), chocolate, nicotine, alcohol, and carminatives.
- Carminatives are volatile oil extracts of plants, most often oils of spearmint and peppermint.
- And, avoid substances that may promote the secretion of acid, which would be present in higher concentrations than normal if refluxed.
- Substances that increase gastric secretions and acid production include alcohol, calcium, decaffeinated and caffeinated coffee, and tea (specifically, methylxanthines).
- Excessive intakes from foods high in calcium such as dairy products, are not recommended. The reason for avoiding excessively high intakes of dairy foods relates to the fact that the amino acids and peptides (generated by digesting the protein in the dairy products) and calcium in dairy products are known to stimulate gastrin release. Although gastrin increases gastroesophageal sphincter pressure, it is also a potent stimulator of hydrochloric acid secretion.
- Also, you want to avoid foods or substances that may irritate an inflamed esophagus.
- Citrus products and other acidic foods or beverages (like coffee).
- Spices (spices such as red and black pepper, nutmeg, cloves, and chili powder).
- Don’t eat close to bedtime.
- Digesting food at night is a hassle and a big mistake. It’s going to raise your body temperature, keeps the gut working, makes it harder to fall asleep, interferes with deep sleep, promotes acid reflux, bloating, and decreases HRV.
- Stop eating at least 4 hours before going to bed.
- Regulate your circadian rhythm.
- Keep a normal sleep schedule by going to bed at the same time every night and waking up at the same time every morning.
- Given the importance of the vagus nerve in the gut (and other organs), when it’s not working right, it will cause digestive disorders including dyspepsia, gastroparesis, esophageal reflux to name a few.
- The vagus nerve is important in conditions like GERD not only because it controls stomach acidity, but also because it controls the esophagus.
- Improve your vagal tone.
- The parasympathic nervous system is responsible for normal digestion (rest and digest). The more stressful our lives, the more the sympathetic nervous system predominates.
- Gargle with water several times a day. The vagus nerve activates the muscles in the back of the throat that allow you to gargle. Gargling contracts these muscles, which activates the vagus nerve and stimulates the gastrointestinal tract. Drink several large glasses of water per day and gargle each sip until you finish the glass of water. You should gargle long enough and deep enough to make it a bit challenging. A two-second light gargle may be equivalent to using a 2-pound dumbbell to strengthen your arm versus a 10-pound dumbbell. It will not work unless it is more challenging. Do this exercise for several weeks to help strengthen the vagal pathways.
- Here’s a list of other activities that can increase parasympathetic nervous system activity:
- Massages
- Aerobic exercise
- Meditation or prayer
- Intermittent fasting
- Sauna
- Cold showers or cold plunge
- Maintaining hydration
- Getting natural light first thing in the morning
- Avoid blue light at night (screens)
- Listening to classical music
- Yoga or Tai Chi practic
- Spending time with friends & family (if they are positive social relationships)
- Practicing gratitude
- Supplements (probiotics, fish oil, CBD)
- Lavender essential oil
- Acupuncture
- Chewing gum
- Laughing
- Breathwork
- Avoid acid blocking agents.
- I really advise against using acid blocking agents because it’s considered counterintuitive to treat GERD with acid blockers because oftentimes people actually need more hydrochloric acid, not less. Low stomach acid can affect lower esophageal tone contributing to reflux.
- This is not true in all cases but more than people realize. Symptoms of hypochlorhydria include: bloating, belching, burning and excessive gas immediately after meals; a sense of fullness even with even smaller meals, indigestion, diarrhea or constipation; food reactions; acne; iron deficiency; chronic or recurrent intestinal parasites and dysbiosis (abnormal gut flora); undigested food in the stool.
- See my HCL protocol to find out if you are a good candidate!
Conclusion
Hopefully this article helps you understand GERD better and learn how to treat it appropriately! I know this causes a lot of pain for a lot of people and it’s no necessary for people to suffer so much. But, healing requires a commitment to change. GERD is curable and you don’t have to resort to acid blockers as your only option. These are linked to dementia, which is why I don’t recommend people take them. If you commit to lifestyle shifts you can experience a lot less GERD!
To learn more about this topic check out the following articles:
- Alternatives to PPIs from the Institute of Functional Medicine
- A Functional Medicine Approach to GERD
- How to Cure GERD Without Medication
If you want more comprehensive guidance on, consider taking my online course, “Your Healthspan Journey” I taught at Stanford for 3 years which is truly the ultimate masterclass in health optimization.
Disclaimer: As an Amazon Associate I earn from qualifying purchases.